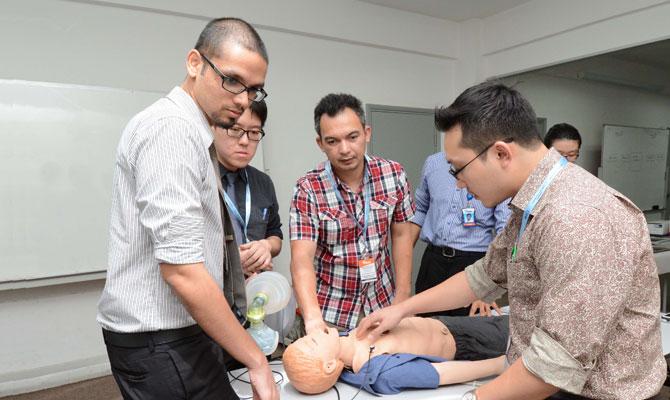
The Clinical Skills & Simulation Centre (CSSC) at the International Medical University (IMU) provides a physical and educational resource in clinical skills learning for health professional programmes within the Faculty of Medical and Health Sciences.
About the Centre
Message from the Director

Dr Juliet Mathew
Director, Clinical Skills and Simulation Centre,
MBBS(Man) MCOUNS (UM)
“Our mission is to establish as a center of excellence for higher education, providing training through multidisciplinary programs. The team at CSSC comprises of a knowledgeable and skillful group of trained professionals with high ethical standards dedicated to serving and improving the quality of life of the community. We aim to support undergraduate and postgraduate health professional students in a simulated clinical environment with the goal of improving the quality of care given to patients in the clinical setting.
Our ultimate vision is to inspire and teach students to learn, review and practise the skills they require, and promote the making of excellent healthcare practitioners of the future.”
What is Direct Observation of Procedural Skills or DOPS?
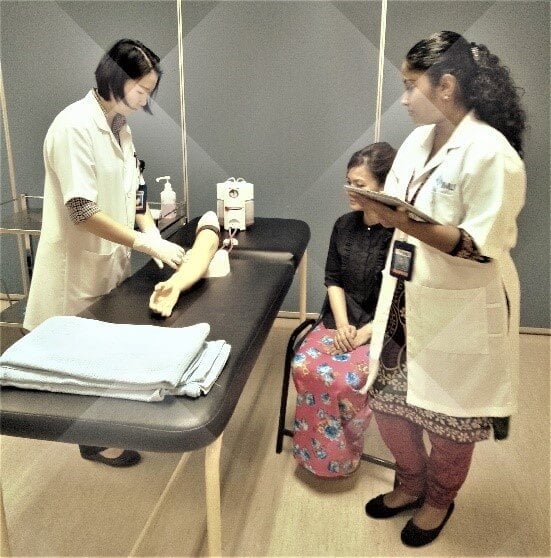
Direct Observation of Procedural Skills or DOPS is a structured assessment for students on their practical procedure competency as well as communication skills with the patient. This is part of a competency assessment required in an undergraduate training. It has been practised worldwide in medical schools and has proven to give a very good outcome. The assessors should be from trained health personnel that requires a standard way of understanding and assessment method. The assessor can be doctors or qualified nurses. Each procedural skill will take approximately 5 minutes, followed by 5 minutes of verbal feedback by the assessor. However, the time allocated depends on the length of the procedure to be carried out. The checklist prepared is based on the standard procedure that is being practised worldwide with an emphasis on patient safety and professionalism. DOPS assessment is included in the students’ log book.
What is Simulated Patient (SP)?

How to Join?
01
You are required to attend a compulsory half-day orientation programme before enrolling as a SP.
02
If you are below 18 years old, your parents are also required to attend the compulsory half-day orientation programme before enrolling as a SP.
03
Fill up the form below
FAQ
Is this a full-time or part-time employment?
No, being an SP is on a voluntary basis. This cannot be considered as a full time/part-time employment. However, a small token of appreciation will be given for each participation.
What about transportation or parking?
Most of the sessions take place at IMU Bukit Jalil. You are advised to park at Bukit Jalil Stadium Carpark B, RM2 will be charged for per entry. You can then take the shuttle bus to IMU. There will be no reimbursement for your parking or transportation fee.
How often would I be scheduled?
During the academic year, SPs are carefully matched to clinical sessions and course requirements. Thus, your schedule is no fixed, can be from 0 -4 or more a month. Scheduling is done at your convenience and is based on the type of session for which you are best suited.
Services and Training
What is The Peer Tutor Programme?

The Peer Tutor Programme started in December 2011 and was initiated by Dr Janet Porter, a Visiting Lecturer from St. George’s University, UK. The concept and evidence for peer teaching have long been part of the medical education programme. It was also created in line with the International Medical University’s Policy for Peer tutoring.
Tutors are recruited on a voluntary basis from cohorts who had recently graduated from the medical programme (after their Semester 10 examination) and cohorts who had completed their First Professional Part 2 Examinations (Semester 5). These group of tutors was found to be most suitable as they were either awaiting their posting into the housemanship or awaiting their transfer to Partner Medical Schools. Thus, they were available to tutor classes during the semester.
All tutors have to attend a mandatory preparatory workshop to equip them with theoretical and practical skills before taking up the role of a tutor.