When compared to other disciplines, the healthcare sciences are unique in that they involve an immense amount of hands-on, practical work that need to be delivered with care and compassion. Working in a high-stress environment that necessitates a high level of technical finesse and punishes even the smallest margin of error is no easy task for even a seasoned veteran, let alone a healthcare student fresh from college or high-school. For this reason, it is imperative that every healthcare education provider does its utmost to provide safe learning spaces that accurately simulate the real-life scenarios healthcare professionals will inevitably face. ‘Realistic but risk-free’ is the mantra at the International Medical University (IMU), where the Clinical Skills and Simulation Centre (CSSC) in particular focuses ample time and resources in developing the best learning experience possible for its students.
Dr Sow Chew Fei, IMU’s CSSC director, stresses that practical work students do with models and simulated patients is arguably as important to the development of competencies of a healthcare professional as the theoretical, knowledge-based concepts of health sciences received during lectures. For this reason, Dr Sow and her team have made great efforts in developing the CSSC to better accommodate student learning needs while also presenting a safe space that provides high fidelity simulations in accordance with accreditation and professional requirements.
One practical hurdle most universities face when it comes to preparing simulation learning is the constraint of space. Given the difficulty of having an entire hospital facility on campus, what with its various departments and rooms, spanning multiple floors, universities need to be innovative in order to give students the full breadth of clinical and communication skill exercises, diverse case scenarios and learning experiences necessary for healthcare professional training. Dr Sow explains that IMU tackles this hurdle by converting rooms to different sizes through the use of collapsing partitions to suit the needs of a particular training session or assessment. That way, a maternity ward, a paediatrician’s room and a chiropractor’s table can all coexist in the same space.
One learning space that is a favourite and commonly utilised by students is the CSSC self-directed learning room containing several booths, each with its own skills based task, allowing students to practice taking blood samples, conducting pap smears or delivering a baby with video guidance. The CSSC team’s video tutorials are painstakingly made in house for each booth, created to be as clear and thorough as possible, allowing students to hop from booth to booth and practice crucial, technical skills that can be applied later in a more safe and comfortable manner on real clients or patients. This practice room is an example of how IMU’s CSSC team cleverly optimises space to make a comfortable learning environment for students, proving that a lack of space is no excuse when it comes to giving students the opportunity to practice a wide range of technical skills.
Dr Sow makes it clear that efficiently running the CSSC requires coordination and cooperation from the whole team. Just as a hospital is a complex ecosystem of people in different roles and departments working together, the CSSC team is similarly diverse, consisting of not only doctors and nurses but also experts in management and administration.
Besides having state of the art models for students to work with, the Simulated and Real Patients team have carefully designed an efficient system where simulated patients are prepped and trained to provide students the most realistic experience of interacting with patients. Developing good bedside manners and being able to determine all the prudent pieces of information from a patient is a crucial skill for any healthcare professional, and well trained simulated patients who can role play challenging and well-developed scripts are a big part of the student’s learning experience. 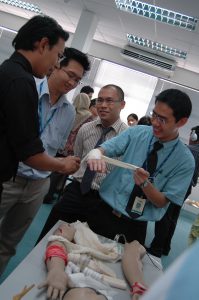 As the patient or client voice is crucial to efficient, safe and compassionate healthcare delivery worldwide, IMU’s CSSC is also benchmarking the training and roles both its simulated and real patients play in the learning environment of healthcare students to international best practices. Visiting professors from IMU’s partner medical schools are continuously engaged for simulated and real patient training, case scenarios development and communication skills assessment. The aim is to ensure that IMU students are also well prepared to transfer to the diverse healthcare setting the partner schools provides. The student response to the CSSC team’s efforts has been very positive. Semester 3 medical students Carmen and Gan tell us about how initially, being introduced to the CSSC can be an intimidating experience. According to Gan, “there are many seemingly complex skills the students are expected to master and it can sometimes feel like being thrown into the deep end.” In the beginning, it is normal to struggle with some procedures, but instead of getting discouraged, Gan tells us he and other students “were able to push through with the help and guidance of friendly CSSC lecturers and tutors.”
As the patient or client voice is crucial to efficient, safe and compassionate healthcare delivery worldwide, IMU’s CSSC is also benchmarking the training and roles both its simulated and real patients play in the learning environment of healthcare students to international best practices. Visiting professors from IMU’s partner medical schools are continuously engaged for simulated and real patient training, case scenarios development and communication skills assessment. The aim is to ensure that IMU students are also well prepared to transfer to the diverse healthcare setting the partner schools provides. The student response to the CSSC team’s efforts has been very positive. Semester 3 medical students Carmen and Gan tell us about how initially, being introduced to the CSSC can be an intimidating experience. According to Gan, “there are many seemingly complex skills the students are expected to master and it can sometimes feel like being thrown into the deep end.” In the beginning, it is normal to struggle with some procedures, but instead of getting discouraged, Gan tells us he and other students “were able to push through with the help and guidance of friendly CSSC lecturers and tutors.”
Carmen says that she and other students were able to practice their skills through IMU’s DOPS (Direct Observation of Procedural Skills) “without any fear of judgment or harsh criticism.” DOPS is an evidence-based assessment that guides students develop competencies in clinical procedural skills. DOPS at IMU allows students to book sessions with their clinical faculty or CSSC tutors and have them supervise the students as they perform a clinical procedure, in order to give guidance and feedback. The DOPS system allows students to practice their skills under the watchful eye of a trained healthcare professional before being formally assessed on their ability or performing on real patients. DOPS is just one example of the varied learning activities at the CSSC which is designed in order to provide students with professional guidance and supervision wherever they may need it, and the positive effects of this design are evident to the students. Professional nurses who are CSSC faculty describe how students can struggle through procedures such as the venal puncture, sometime feeling hesitant to the thought of using needles. Through scheduled and non-scheduled learning times, students are able to iron out these hurdles through the mentorship of the faculty and progress in their developing their clinical and communication skills. As IMU is big on incorporating personalised learning into various aspect of its curriculum, the training at the CSSC is no exception. Dr Sow warns of a trend amongst healthcare education providers to invest heavily in an abundance of teaching models of the highest calibre, only to restrict student access to such models for fear of damaging them. She says this kind of thinking not only puts the expensive resources to waste, but it also underestimates and infantilises medical students and their ability to be cautious with equipment. 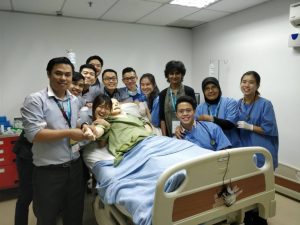 Limiting student use of models and equipment at the CSSC to the close supervision of teachers is unnecessary, says Dr Sow, so long as the students are well-informed as to the correct practices. Allowing students the freedom to book appointment slots in order to practice technical skills with models really enables them to take their learning and preparation into their own hands, and will also allow them to prepare better for assessments. Students can log in practice hours in groups, allowing them to get a grasp on the collaborative aspect of healthcare services, and allowing group mates to help and guide one another in accomplishing certain tasks.
Limiting student use of models and equipment at the CSSC to the close supervision of teachers is unnecessary, says Dr Sow, so long as the students are well-informed as to the correct practices. Allowing students the freedom to book appointment slots in order to practice technical skills with models really enables them to take their learning and preparation into their own hands, and will also allow them to prepare better for assessments. Students can log in practice hours in groups, allowing them to get a grasp on the collaborative aspect of healthcare services, and allowing group mates to help and guide one another in accomplishing certain tasks.
Students agree that the independent route to learning is best – they feel that without that level of trust from the CSSC team they wouldn’t be able to develop a sense of responsibility and confidence in their work. Students can see that the principles at the CSSC, from the independent learning slots to the enforced dress code that mimics hospital attire, encourages a degree of professionalism that can only be beneficial in the long run. Students also appreciate the high fidelity models prepared to give them the most realistic learning experience possible. Some of the models can breathe and talk.
Certain mock surgery or patient rooms have one sided observation glass, allowing staff to sit in a panel on the other side and adjust conditions as necessary in order to challenge the students. Dr Sow shares humorous anecdotes about how the models are manipulated based on scenarios to stop breathing or flatline in the middle of a procedure, right when students have gotten comfortable, in order to keep them vigilant and help them manage their panic in stressful situations. It is evident that the CSSC is multi-faceted in its approach to teaching and learning, making efforts to provide the most holistic technical training possible within finite resources. Just as the field of healthcare is constantly changing and adapting, the CSSC at IMU is also in a constant state of evolution, forever growing and changing to suit the learning needs of future healthcare professionals.




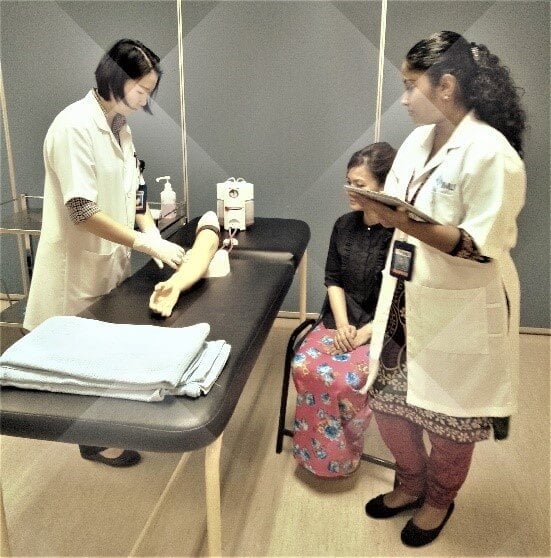 Clinical Skills and Simulation Centre
Clinical Skills and Simulation Centre 






